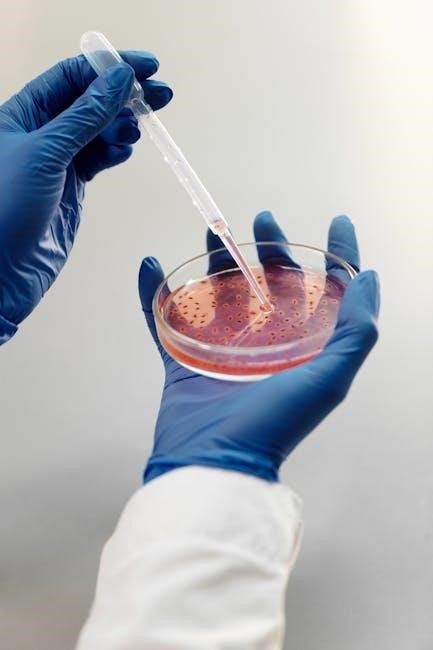
microbiology laboratory theory and application pdf
Microbiology laboratory manuals, like the 10th edition by James, and practical guides detail essential techniques.
These resources cover sterilization, culturing, and identification methods, aiding comprehensive understanding.
What is Microbiology?
Microbiology is the study of microscopic organisms – bacteria, viruses, fungi, and protozoa – and their activities. It’s a broad discipline encompassing their roles in disease, environment, and industry. Laboratory manuals, such as those referenced (Harley’s and the 10th edition), provide foundational theory and practical application.
These texts detail techniques for observing, isolating, and identifying these organisms. Understanding microbial morphology, employing staining like acid-fast, and mastering culturing (streak/pour plates) are core components. The field’s relevance spans clinical diagnostics, environmental monitoring, and biotechnological advancements, all underpinned by robust laboratory practices.
Importance of Microbiology Laboratories
Microbiology laboratories are crucial for diagnosing infectious diseases, monitoring environmental quality, and advancing biotechnological research. Manuals like the “Manual of Clinical Microbiology” (Murray) emphasize their diagnostic role. Accurate identification, utilizing biochemical tests and microscopic examination, directly impacts patient care.
Furthermore, labs support public health by tracking outbreaks and antibiotic resistance. Industrial microbiology relies on labs for strain development and quality control. Effective lab practices, detailed in comprehensive guides, ensure reliable results and safe handling of potentially hazardous materials, underpinning advancements across diverse scientific fields.

Essential Laboratory Equipment
Essential tools include microscopes for visualization, autoclaves for sterilization, and incubators for controlled growth – all detailed within microbiology laboratory manuals and guides.
Microscopes and Their Types
Microscopes are fundamental to microbiology, enabling visualization of microorganisms. Various types exist, each with unique capabilities. Bright-field microscopy, the most common, provides direct illumination. Phase-contrast microscopy enhances contrast for observing live, unstained specimens. Dark-field microscopy illuminates specimens against a dark background, ideal for observing motility.
Furthermore, fluorescence microscopy utilizes fluorescent dyes to highlight specific structures. Electron microscopy, offering significantly higher resolution, reveals ultrastructural details. Laboratory manuals, such as those referenced, comprehensively detail these microscope types, their principles, and appropriate applications in microbiological studies. Proper microscope usage is crucial for accurate identification and analysis.
Autoclaves and Sterilization
Sterilization is paramount in microbiology to eliminate all microbial life. Autoclaves achieve this using high-pressure steam, typically 121°C for 15-20 minutes. This method effectively destroys bacterial spores, viruses, and fungi. Laboratory manuals emphasize proper loading techniques to ensure steam penetration.
Other sterilization methods include dry heat sterilization and filtration. However, autoclaving remains the gold standard for many laboratory applications. Understanding autoclave principles, including pressure, temperature, and time, is vital. Quality control measures, like biological indicators, verify sterilization efficacy, as detailed in microbiology laboratory guides.
Incubators and Temperature Control
Incubators provide controlled environments for microbial growth, maintaining optimal temperature, humidity, and often CO2 levels. Most bacteria thrive at 37°C, mimicking the human body, while others require different temperatures. Precise temperature control is crucial for consistent results.
Microbiology laboratory manuals highlight the importance of incubator calibration and monitoring. Temperature fluctuations can significantly impact growth rates and metabolic processes. Some organisms need anaerobic conditions, requiring specialized incubators. Regular maintenance and proper usage are essential for reliable microbial cultures, as detailed in practical microbiology guides.

Sterilization and Disinfection Techniques
Sterilization, like autoclaving and pasteurization, eliminates all microbes, while disinfection reduces their numbers. Manuals emphasize safe disinfectant usage and proper procedures.
Autoclaving Principles and Procedures
Autoclaving utilizes high-pressure steam to achieve sterilization, effectively eliminating microorganisms and spores. The principle relies on moist heat denaturing proteins and destroying microbial structures. Proper procedures, detailed in laboratory manuals, involve loading materials correctly, ensuring adequate steam penetration, and monitoring temperature and pressure.
Typically, autoclaving occurs at 121°C (250°F) for 15-20 minutes, though times vary based on load volume and material type. Successful autoclaving requires validation using biological indicators, like Geobacillus stearothermophilus spores, to confirm sterilization effectiveness. Safety protocols are crucial, including cautious unloading to avoid burns from hot materials and steam.
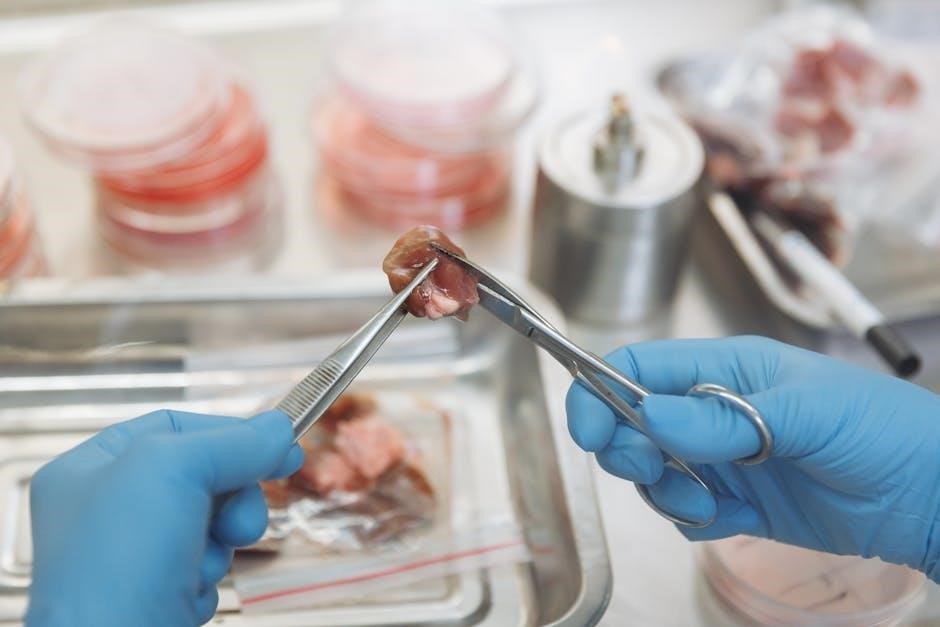
Pasteurization Methods
Pasteurization is a heat treatment applied to liquids, primarily food and beverages, to eliminate pathogenic microorganisms and reduce spoilage organisms. Unlike sterilization, it doesn’t aim for complete microbial destruction, but rather reduces the microbial load to safe levels. Several methods exist, including High-Temperature Short-Time (HTST) – 72°C for 15 seconds – and Ultra-High Temperature (UHT) – 135-150°C for a few seconds.
Laboratory manuals detail these processes, emphasizing their application in controlling microbial growth in various products. Pasteurization extends shelf life and ensures product safety, though some heat-resistant spores may survive. It’s a critical technique in food microbiology and quality control.
Disinfectant Usage and Safety
Disinfectants are crucial for controlling microbial growth on inanimate surfaces, differing from antiseptics used on living tissue. Laboratory manuals emphasize proper usage, including dilution, contact time, and compatibility with materials. Common disinfectants include bleach, alcohol, and quaternary ammonium compounds, each with specific efficacy against different microorganisms.
Safety is paramount; always wear appropriate personal protective equipment (PPE) – gloves, eye protection, and lab coats – when handling disinfectants. Proper ventilation is essential, and disposal must follow established protocols to prevent environmental contamination. Understanding disinfectant limitations is vital for effective microbial control.

Culture Media Preparation
Culture media, including nutrient, selective, and differential types, are fundamental for microbial growth. Manuals detail agar preparation, sterilization, storage, and quality control procedures.
Types of Culture Media (Nutrient, Selective, Differential)
Microbiology laboratories utilize diverse culture media tailored to specific microbial needs. Nutrient media provides basic nourishment for general growth, supporting a wide range of organisms. Selective media incorporates components that inhibit the growth of certain microbes while promoting others, aiding in isolation.
Differential media contains indicators to visually distinguish between different microbial groups based on metabolic characteristics. These distinctions are crucial for identification. Manuals emphasize proper media selection based on the target organism and experimental goals, ensuring accurate results and efficient laboratory workflows. Understanding these types is fundamental to successful microbial cultivation.
Agar Preparation and Sterilization
Agar, a polysaccharide derived from seaweed, is a crucial solidifying agent in microbiological media. Accurate weighing and dissolving of agar in the appropriate liquid medium are essential for consistent results. Following dissolution, sterilization is paramount, typically achieved through autoclaving – utilizing high-pressure steam to eliminate all microorganisms.
Manuals detail specific autoclaving parameters (temperature, pressure, time) to ensure complete sterilization without degrading the agar’s properties. Proper sterilization prevents contamination and ensures reliable culture growth. Quality control checks, like visual inspection for turbidity, confirm media sterility before use, upholding laboratory standards.
Media Storage and Quality Control
Prepared media requires careful storage to maintain viability and prevent contamination. Typically, sealed petri dishes and tubes are stored inverted in a cool, dark place, minimizing moisture loss and light-induced degradation. Quality control is vital; sterility checks before and after storage are essential, observing for turbidity or growth.
Periodic testing with known organisms confirms media performance – ensuring proper growth promotion and differential characteristics. Documentation of storage conditions and QC results is crucial for traceability and reliable experimental outcomes, as detailed in microbiology laboratory manuals.

Basic Microbiological Techniques
Essential techniques include smear preparation, heat fixing, and staining – Gram and acid-fast – alongside culturing methods like streak and pour plates, as detailed in manuals.
Smear Preparation and Heat Fixing
Smear preparation is a foundational microbiology technique, initiating the microscopic examination of microorganisms. A small sample is spread thinly on a slide, ensuring individual cells are discernible.
Heat fixing then secures these cells to the slide, preventing washing away during staining procedures. This involves briefly passing the slide through a flame, coagulating proteins and adhering the microbes.
Manuals, such as those referenced, emphasize proper heat fixing – avoiding excessive heat which can distort cellular morphology. Correctly prepared and fixed smears are crucial for accurate staining and subsequent identification, forming the basis for many laboratory analyses.
Staining Techniques (Gram Stain, Acid-Fast Stain)
Staining enhances microbial visibility under a microscope, revealing crucial structural details. The Gram stain, a differential stain, categorizes bacteria into Gram-positive and Gram-negative based on cell wall composition. Manuals detail the four-step procedure – primary stain, mordant, decolorizer, and counterstain – for accurate differentiation.
The acid-fast stain identifies bacteria with waxy mycolic acids in their cell walls, like Mycobacterium. This technique utilizes carbolfuchsin and a decolorizer, resisting removal from acid-fast cells. Proper technique, as outlined in laboratory guides, is vital for reliable results.

Culturing Techniques (Streak Plate, Pour Plate)
Culturing techniques are fundamental for isolating and growing microorganisms. The streak plate method aims to obtain isolated colonies from a mixed culture, diluting bacteria across an agar surface. Laboratory manuals illustrate proper streaking patterns for effective separation.
The pour plate technique involves mixing a diluted sample with molten agar before pouring into a petri dish. Colonies grow both on and within the agar. These methods, detailed in microbiology guides, require aseptic technique to prevent contamination and ensure accurate representation of the original sample.
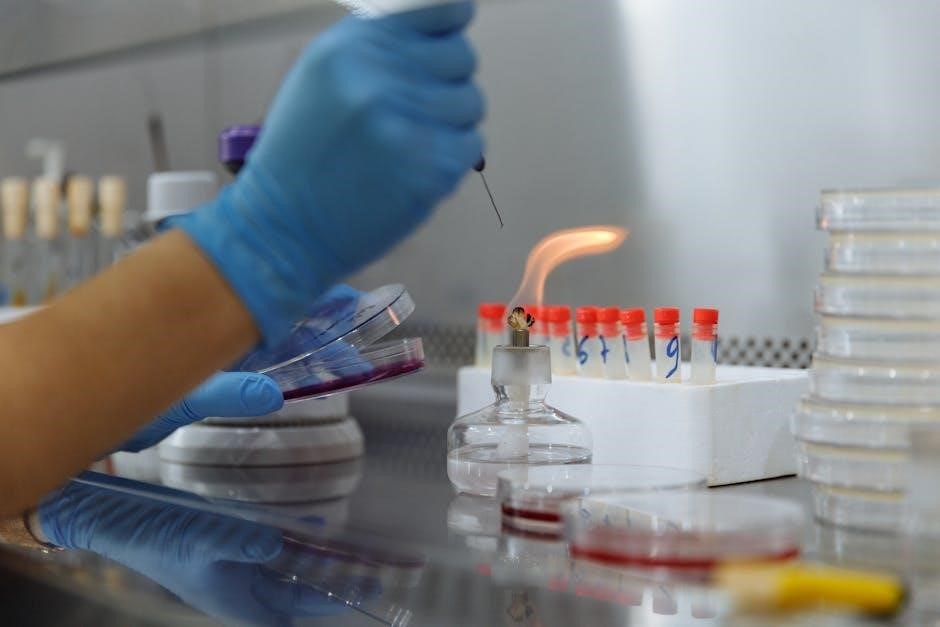
Microbial Identification Methods
Microbial identification utilizes biochemical tests, microscopic examination of cellular morphology, and increasingly, molecular techniques as detailed in lab manuals.
Biochemical Tests for Identification
Biochemical tests are fundamental in microbiology for identifying bacteria based on their metabolic capabilities. These tests assess an organism’s ability to utilize specific substrates, produce enzymes, or generate certain end products.
Common examples, often detailed in laboratory manuals like those referenced, include catalase, oxidase, and various fermentation tests. These assays help differentiate between closely related species.
The results are interpreted according to standardized charts, allowing for accurate identification. Manuals provide protocols and expected outcomes, crucial for reliable diagnostic microbiology and research applications.
Microscopic Examination of Cellular Morphology
Microscopic examination remains a cornerstone of microbial identification, allowing direct observation of cellular shapes, arrangements, and structures. Laboratory manuals, such as those detailing techniques for smear preparation and staining, emphasize this crucial step.
Techniques like Gram staining, and acid-fast staining, detailed in referenced PDFs, differentiate bacteria based on cell wall properties. Observing morphology aids in preliminary identification and guides further biochemical testing.
Detailed manuals provide guidance on proper slide preparation and interpretation of microscopic findings, essential for accurate and reliable results in clinical and research settings.
Molecular Techniques in Microbial Identification
Modern microbiology increasingly relies on molecular techniques for precise microbial identification, supplementing traditional methods. Referenced PDFs highlight the growing role of these advanced approaches in clinical and research laboratories.
These techniques, often detailed in comprehensive manuals, include PCR-based assays, DNA sequencing, and other methods to analyze microbial genomes directly. This allows for rapid and accurate identification, even for difficult-to-culture organisms.
Molecular methods offer enhanced sensitivity and specificity, crucial for detecting pathogens and understanding microbial diversity, as detailed in resources like the Manual of Clinical Microbiology.

Safety Protocols in the Microbiology Lab
Essential lab manuals emphasize biosafety levels, handling infectious materials, and proper waste disposal procedures. These protocols ensure a safe working environment.
Biosafety Levels and Practices
Microbiology laboratories adhere to a tiered biosafety level system – from BSL-1, suitable for introductory training, to BSL-4, handling dangerous and exotic agents. Manuals detail specific practices for each level, including required personal protective equipment (PPE) like gloves and lab coats.
Standard microbiological practices are crucial, encompassing safe handling of cultures, proper disinfection of work surfaces, and meticulous handwashing. These practices minimize exposure risks. Furthermore, manuals emphasize the importance of risk assessments before commencing any experiment, ensuring appropriate containment measures are in place to protect personnel and the environment.
Handling of Infectious Materials
Microbiology laboratory manuals emphasize stringent protocols for handling potentially infectious materials. This includes careful labeling of all cultures and specimens with appropriate biohazard warnings. Aseptic techniques are paramount to prevent contamination and accidental exposure.
Detailed procedures outline the safe transfer of cultures, proper use of biological safety cabinets, and immediate decontamination of spills. Personnel must be thoroughly trained in these procedures. Manuals also stress the importance of minimizing aerosol production and avoiding direct contact with infectious agents, safeguarding both researchers and the surrounding environment.
Waste Disposal Procedures
Microbiology laboratory manuals dedicate significant sections to proper waste disposal, crucial for preventing the spread of infection. All contaminated materials – cultures, petri dishes, swabs – must be autoclaved before disposal to ensure complete sterilization.
Sharps, like needles and slides, require separate, puncture-proof containers. Liquid waste often necessitates chemical disinfection before being poured down the drain, adhering to local regulations. Detailed protocols outline segregation of waste streams, proper container labeling, and adherence to biosafety level guidelines, minimizing environmental and health risks.

Applications of Microbiology Laboratory Techniques
Microbiology techniques find broad application in clinical diagnostics, environmental monitoring, and industrial biotechnology, as detailed in manuals and practical guides.
Clinical Microbiology and Diagnostics
Clinical microbiology heavily relies on laboratory techniques outlined in resources like the Manual of Clinical Microbiology. These techniques are crucial for identifying pathogenic microorganisms causing infectious diseases. Diagnostic procedures encompass bacterial culture, staining (Gram stain, acid-fast stain), and biochemical testing to determine antibiotic susceptibility.
Molecular techniques, increasingly important, aid in rapid and accurate identification. Labs apply these methods for diagnosing infections, guiding treatment strategies, and monitoring disease outbreaks. Manuals provide detailed protocols for safe handling of infectious materials and proper waste disposal, ensuring accurate patient care and public health protection.
Environmental Microbiology and Monitoring
Environmental microbiology utilizes laboratory techniques to assess microbial populations in diverse ecosystems – water, soil, and air. Manuals detail methods for monitoring environmental quality, detecting pollutants, and evaluating the impact of human activities. Culturing techniques, like streak plates and pour plates, are employed to isolate and identify microorganisms.
These labs analyze microbial indicators of contamination, assess bioremediation potential, and monitor water safety. Techniques from microbiology laboratory manuals are vital for ensuring environmental health, protecting ecosystems, and safeguarding public well-being through informed monitoring and assessment strategies.
Industrial Microbiology and Biotechnology
Industrial microbiology leverages microbial processes for large-scale production, relying heavily on laboratory techniques detailed in manuals like those by Harley. These techniques encompass strain improvement, fermentation optimization, and product recovery. Microbiology labs are crucial for quality control in industries like food, pharmaceuticals, and biofuels.
Biotechnology applications, such as enzyme production and genetic engineering, depend on precise microbial culturing and analysis. Manuals guide biochemical tests for identifying industrially valuable strains and monitoring their performance. These lab skills are fundamental for innovation and efficiency in biotechnological processes.
Leave a Reply
You must be logged in to post a comment.